septembre 16, 2017
9 Facts About Fertility You Should Learn In Your Twenties
9 Facts About Fertility You Should Learn In Your Twenties
1. There is a drop-off in fertility, especially for women, as you get older. But it might not be as dramatic as you think.

Halfpoint / Getty Images
If you're a woman, your chance of conceiving each time you have unprotected sex starts to drop in about your mid-thirties. But media reports of a "fertility cliff" are overblown.
"There certainly is a reduction in female fertility in age," Tim Child, a consultant gynaecologist and professor at the University of Oxford, tells BuzzFeed News. "But it's certainly not a cliff. It's a gradual decline that steepens as you get towards your late thirties." A couple where the woman is 40 "has about a 50% chance of conceiving" in 12 months of trying, he says, although the risk of miscarriage is higher.
Robert Winston, an emeritus professor of fertility studies at Imperial College London, agrees. "Women are more fertile than they realise, for a long time," he tells BuzzFeed News. "The average age of having your first baby is over 30 now, and there isn't any decrease in national fertility that we can see. So the idea that you are becoming infertile at 30 is nonsense."
2. If you're trying to conceive and don't get pregnant right away, you really don't need to worry.
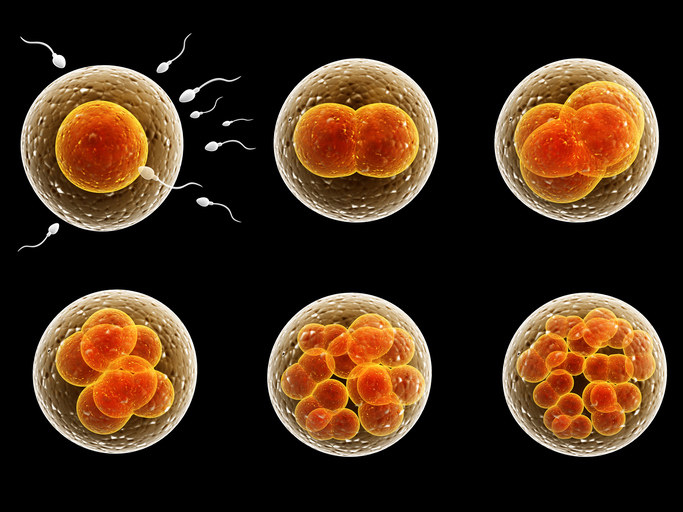
Frentusha / Getty Images
If you're trying to get pregnant, each month that passes can feel incredibly long. But it's pretty rare to get pregnant straight away.
"The chance of a British couple getting pregnant each cycle is about 20%," says Winston. "It's a bit higher in Australia, where people have a bit more sex; it's a bit lower in France, where people have less.
"So on average, it takes five months to get pregnant. You're not unusual unless you've gone 10 months or a year. I wouldn't dream of examining someone until it's been a year, unless there was some specific reason you thought there was a problem."
Dr Helen Munro, a sexual and reproductive health consultant, agrees. "If a couple have been having sex two or three times a week for a year and still not fallen pregnant, they'd be the ones I'd look at," she told BuzzFeed News. "Otherwise, you're fertile until proven otherwise."
Child says "the chances of a healthy couple conceiving in a year is about 80%, and importantly, half of the ones who haven't will conceive naturally the year after. Often it just takes longer."
3. Contraception can't make you infertile.
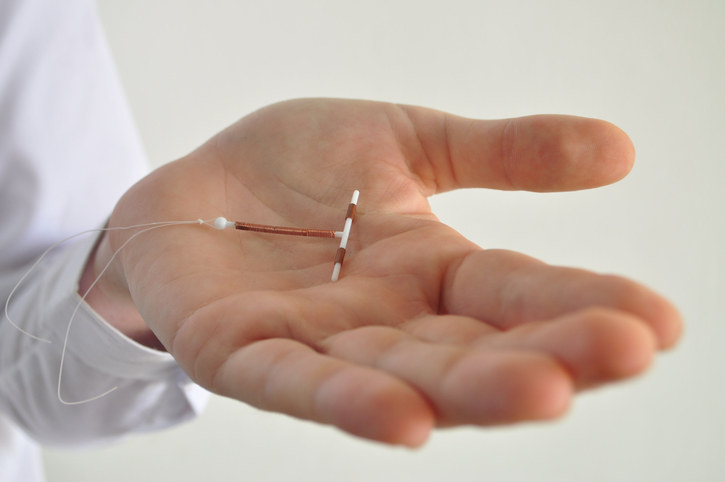
Flocu / Getty Images
"The number one thing with our female patients starting contraception is they have these ideas about contraception causing infertility. The pill making you infertile, or a coil making you infertile," says Munro.
"I spend a lot of time reassuring young women that contraception can't make you infertile. The myths are maybe from people who've come off contraception and then struggle to get pregnant, but it's not to do with the contraception. As a doctor, I want to first do no harm. If there was any reason we thought that contraception could cause infertility, that would be harm, and I couldn't do it."
4. Your risks of failing to conceive and of miscarriage increase into your late thirties and forties.
![Women are born with between 2 million and 3 million eggs in their ovaries, says Child. "The common myth is that [you become infertile when] you run out of eggs," he says. "Occasionally that's the case, but generally it's that as you get older, the eggs that remain are of poorer quality. We don't really know why." So you may continue ovulating, but your eggs are more likely to have genetic problems. That means that if they're fertilised, they're less likely to implant, and if they do implant, you're more likely to have a miscarriage further along in the pregnancy.How late you want to leave it depends on lots of things. "We're living longer and working longer," says Munro. "We have different priorities – our priority isn't having a baby at 21, and that's a good thing. But our bodies haven't changed. We're still at peak fertility in our mid-twenties." Adam Balen, a consultant in reproductive medicine and chair of the British Fertility Society, says that if you want a "really good" chance of having a larger family, it is better to start earlier. "If you just want one, you can probably wait until your early thirties and still have a really good chance," he tells BuzzFeed News. But if you want more than that, to give yourself the best shot, he says, it may be worth considering starting earlier.But, Munro says, media focus on this can be unhelpful. "Women are inherently aware. We know this and don't need to be told," she says. "As clinicians, we'll work with the choices of the woman, so if she's busy in her career at age 35 and doesn't want an unplanned pregnancy, I'll give her options for good contraception."](https://img.buzzfeed.com/buzzfeed-static/static/2017-09/12/11/asset/buzzfeed-prod-fastlane-03/sub-buzz-5598-1505229731-1.jpg)
Monkeybusinessimages / Getty Images
Women are born with between 2 million and 3 million eggs in their ovaries, says Child. "The common myth is that [you become infertile when] you run out of eggs," he says. "Occasionally that's the case, but generally it's that as you get older, the eggs that remain are of poorer quality. We don't really know why."
So you may continue ovulating, but your eggs are more likely to have genetic problems. That means that if they're fertilised, they're less likely to implant, and if they do implant, you're more likely to have a miscarriage further along in the pregnancy.
How late you want to leave it depends on lots of things. "We're living longer and working longer," says Munro. "We have different priorities – our priority isn't having a baby at 21, and that's a good thing. But our bodies haven't changed. We're still at peak fertility in our mid-twenties."
Adam Balen, a consultant in reproductive medicine and chair of the British Fertility Society, says that if you want a "really good" chance of having a larger family, it is better to start earlier. "If you just want one, you can probably wait until your early thirties and still have a really good chance," he tells BuzzFeed News. But if you want more than that, to give yourself the best shot, he says, it may be worth considering starting earlier.
But, Munro says, media focus on this can be unhelpful. "Women are inherently aware. We know this and don't need to be told," she says. "As clinicians, we'll work with the choices of the woman, so if she's busy in her career at age 35 and doesn't want an unplanned pregnancy, I'll give her options for good contraception."
5. Men's fertility declines as they get older too.
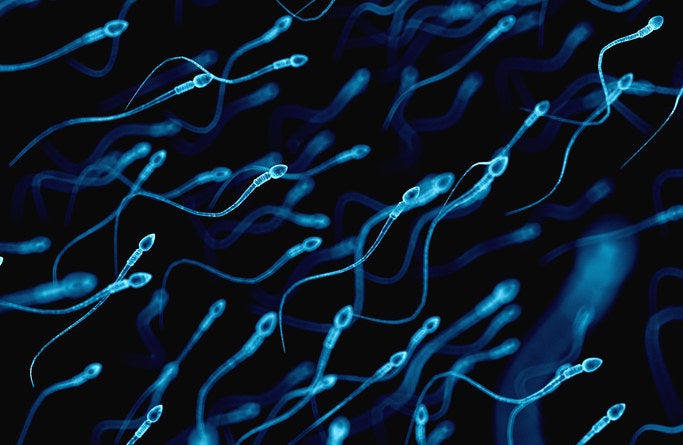
Eraxion / Getty Images
Although the focus is usually on a woman's decline in fertility, there is one for men too. However, it is later and manifests differently.
"The proportion of sperm that have the wrong number of chromosomes goes up, although it's about 10 years later than for women," says Child. "Sperm donors have to be less than 40 in the UK. And for men, even though sperm quality declines, it doesn't go down to zero – so you get the Charlie Chaplins having children in their seventies."
6. IVF isn't a cure-all, and sometimes people might be pushed towards it when they don't need it.
![Winston estimates that half of the IVF cycles given in the UK are unnecessary. "Clinics make money from giving people IVF," he says. That's not to say that lots of couples don't need it, but there is an incentive for the people running clinics to encourage you to use it. Often, he says, specific fertility problems are best treated with specific solutions. "For example, failure to ovulate is better treated with drugs than with IVF," he says. "People with obstructions are better treated with a laparoscopy [keyhole surgery] than with IVF." And if there's no specific cause detected, he says, "you're more likely to get pregnant having sex on the hearth rug" than by undergoing IVF.](https://img.buzzfeed.com/buzzfeed-static/static/2017-09/7/9/asset/buzzfeed-prod-fastlane-03/sub-buzz-30087-1504791829-1.jpg)
Yurkoman / Getty Images
Winston estimates that half of the IVF cycles given in the UK are unnecessary. "Clinics make money from giving people IVF," he says. That's not to say that lots of couples don't need it, but there is an incentive for the people running clinics to encourage you to use it.
Often, he says, specific fertility problems are best treated with specific solutions. "For example, failure to ovulate is better treated with drugs than with IVF," he says. "People with obstructions are better treated with a laparoscopy [keyhole surgery] than with IVF."
And if there's no specific cause detected, he says, "you're more likely to get pregnant having sex on the hearth rug" than by undergoing IVF.
7. Lifestyle can affect a couple's chances of getting pregnant – but, again, probably less than you think.
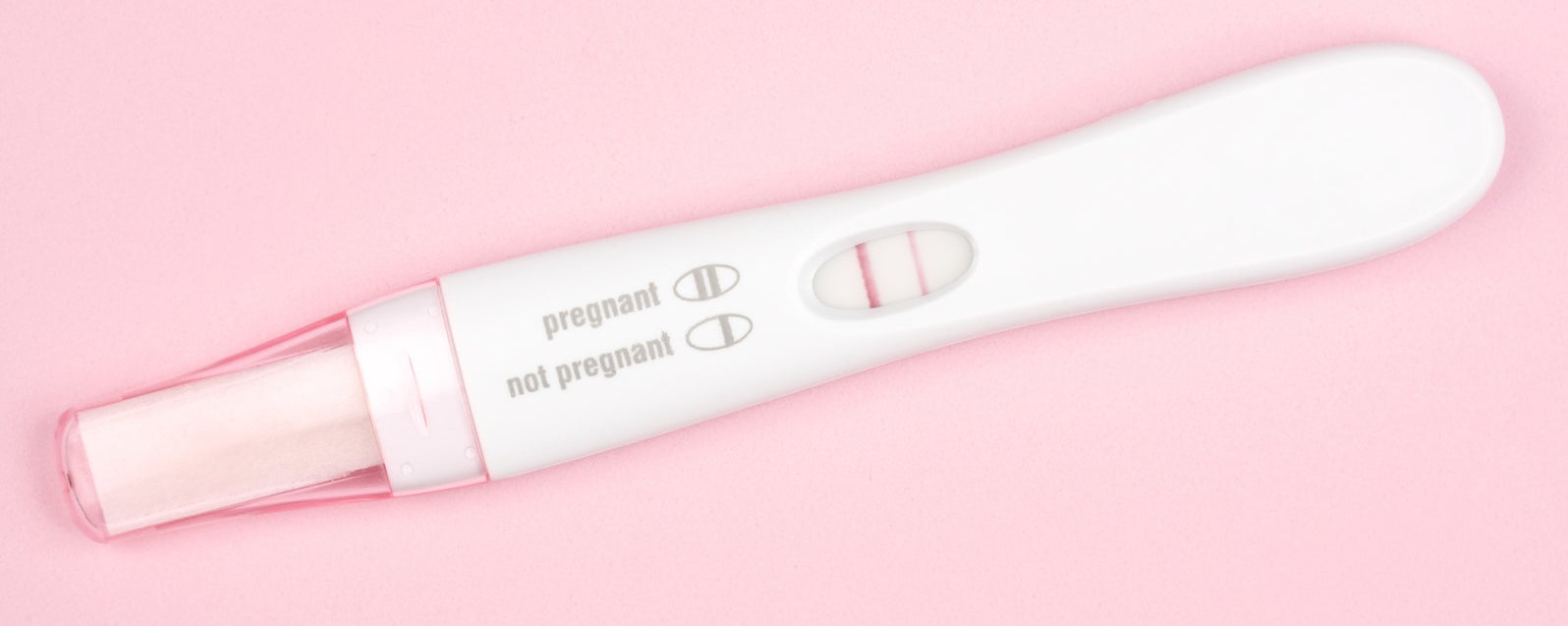
Cillay / Getty Images
"The two things that are proven to reduce fertility are obesity and smoking," says Child. That's true for both men and women, although more so for women.
But the link isn't all that strong. People who smoke and people who are overweight aren't that much less likely to get pregnant than the rest of the population. "You're told that if you smoke a cigarette you'll be infertile, and if you smoke excessively it might reduce your sperm count, but all these lifestyle choices probably don't make a massive difference," says Winston. And the evidence of any effect of alcohol and caffeine on fertility is fairly weak.
It is true that women who are on the very extreme end of physical fitness sometimes stop having periods. "Some female athletes do stop ovulating," says Winston. "But for most young people, that's irrelevant."
8. Although you should probably avoid bodybuilding supplements (not just steroids) and be wary of STIs.
Ugurhan / Getty Images
"It's good to be fit and healthy and go to the gym, but don't use supplements that you get online," says Balen.
That's especially true for ones that you know contain anabolic steroids, he says, but others can also "cause permanent damage to sperm production, so you look muscular but you can turn off sperm production altogether."
"I've seen men with problems with sperm count who say they haven't used steroids but have used supplements," says Balen. "You just don't know what's in them."
Also, some sexually transmitted infections can cause infertility later in life. "Things like chlamydia can increase your chances of fertility problems," says Munro. "If someone's had pelvic inflammatory disease, which can come after untreated chlamydia, I would say you have to be careful because it can affect your fertility. Or if men have gonorrhoea which spread to the epididymis, that can affect sperm production."
9. You can get pregnant later in life than you realise, so don't assume you don't need to worry about contraception when you hit 35.

Jpwallet / Getty Images
The rate of pregnancies among younger women is going down, but it's going up among the over-35s and over-40s. "The question I ask students is: 'Are these unplanned pregnancies, or through choice?'" says Munro. "And I think it's a mix."
She thinks a lot of women assume that because they're over 40 they don't need to worry about contraception any more. "Maybe they're coming out of their first relationships and are navigating sex and relationships at a later age," she says. "Over-40s can get pregnant, absolutely. It's not unheard of for women to forget that because they're told so much about the 'cliff'."
She points to Cherie Blair, who famously got pregnant at 45 while her husband Tony was in office as prime minister. "Until you absolutely stop having periods, you still could be fertile," she says.











![Fertility awareness, also called natural family planning, involves paying attention to signs of fertility like body temperature and cervical secretions. There are apps these days that will help you track signs of fertility, but experts still recommend you get trained by a qualified teacher if you want to use this method."Some women use fertility awareness methods forever and do really well with it," says Connolly. "But you've got to be very disciplined, and your partner's got to be very disciplined."The idea is that by working out when you ovulate, and by knowing that sperm can survive for several days, you can work out when you're fertile and when you're not. On your fertile days, you have to avoid sex or use another method of contraception like condoms. The majority of women ovulate mid-cycle. "But not everyone ovulates when we think they're going to – some women do at any point during the cycle," says Connolly, which can make it tricky to accurately work out your fertile window."It's a method that some people will use reliably, but there's a much higher failure rate [than other forms of contraception]," she says.](https://img.buzzfeed.com/buzzfeed-static/static/2017-09/14/9/asset/buzzfeed-prod-fastlane-03/sub-buzz-11508-1505394107-1.png)
!["Female sterilisation failure rates are actually higher than some forms of contraception, like the Mirena [hormone coil], the copper coil, the implant and the injection," says Connolly.If you're in a monogamous relationship with a male partner and you both know you never want children, vasectomy is another option that may be better from a medical point of view, says Connolly."A vasectomy is 10 times more reliable than female sterilisation," she says. While 1 woman in 200 will become pregnant in her lifetime after being sterilised, only 1 in 2,000 men who have a vasectomy will get a woman pregnant after the operation.She also points out the extra benefits for some women of hormonal methods of contraception: "Sometimes we see women who are sterilised and 10 years down the line they come in with heavy periods so I put a Mirena in."But if you are really sure about wanting sterilisation, your doctor will need to explain the risks to you and make sure you're aware that you're making a decision from here on in. They'll probably also recommend you have counselling before they refer you for the operation.](https://img.buzzfeed.com/buzzfeed-static/static/2017-09/14/9/asset/buzzfeed-prod-fastlane-03/sub-buzz-11560-1505394990-7.jpg)
![Your doctor wants you to feel comfortable and able to talk openly. "Some people are worried, especially if they live in a small community, that family members will find out. But people would lose their jobs [if they told anyone what you'd said]," says Connolly.](https://img.buzzfeed.com/buzzfeed-static/static/2017-09/14/9/asset/buzzfeed-prod-fastlane-02/sub-buzz-16667-1505395383-7.jpg?crop=1596:933;0,216)

